- SPECIALIST ORTHOPAEDIC SURGEON | MELBOURNE, VIC | ALBURY, NSW | MORNINGTON, VIC |
- 03 9421 6133
Total Hip Replacement Surgery
Specialist surgical care for hip arthritis and joint deterioration
Total hip replacement surgery is a highly effective procedure that removes the damaged parts of the hip joint and replaces them with smooth, artificial components. The aim is to reduce pain, restore function, and improve your quality of life.
The information here is designed to help you understand everything involved in hip replacement surgery, including symptoms to look out for, how the procedure works, what recovery involves, and how Dr Jason Hockings personalises care based on your needs.

Could a hip replacement help you move more comfortably?
If you’re living with ongoing hip pain, stiffness, or difficulty walking, you may have already started adjusting your daily life. Many people begin limiting their activity, taking regular pain medication, or avoiding movements that aggravate the discomfort. When non-surgical treatments are no longer providing relief however, total hip replacement surgery may be considered to help improve mobility and reduce pain. This procedure involves replacing the damaged parts of the hip joint with smooth, artificial components. The aim is to create a more comfortable, stable joint that supports better movement and function.
The Aim of Total Hip Replacement Surgery
- Relieve chronic pain that has not responded to other treatments
- Improve walking ability and movement
- Reduce reliance on walking aids such as canes or crutches
- Support a return to daily activities and low-impact exercise
For many patients, the improvement in comfort and mobility allows them to regain independence and participate more fully in work, family life, and recreational activities.
How Hip Joint Damage Affects Movement
The hip is a ball-and-socket joint that plays a major role in weight-bearing and mobility. When the smooth cartilage that lines the joint wears away, the bones can start to rub against each other. This often leads to:
- Groin, buttock, or thigh pain when walking or standing
- Stiffness when getting out of a chair or bed
- A shorter stride or noticeable limp
- Difficulty managing stairs or putting on shoes
- Reduced ability to complete daily tasks independently
Symptoms may progress gradually over time, sometimes becoming more noticeable after periods of rest or increased activity.
Dr Hockings takes a considered, individualised approach to each patient. Not everyone with hip pain requires surgery, and many people benefit from non-surgical management for a period of time. If imaging confirms advanced joint damage and you are finding that pain or stiffness is interfering with your quality of life, hip replacement may be an appropriate next step.
During your consultation, Dr Hockings will assess your condition, review your medical imaging, and discuss whether a total hip replacement may help you move more comfortably and confidently again.
Common signs and symptoms that you may have arthritis

Hip arthritis often develops slowly, and its early symptoms are sometimes mistaken for muscle strain, back issues, or simple fatigue. Over time, as the joint becomes more worn and inflamed, the discomfort tends to become more persistent and starts interfering with everyday activities.
The most common form is osteoarthritis, but symptoms may also arise from rheumatoid arthritis, avascular necrosis, or past injury to the joint. While the underlying causes differ, the signs that suggest hip arthritis are often similar.
Symptoms that may indicate arthritis of the hip:
Pain in the groin, buttock, or thigh
This discomfort is usually felt deep in the joint and may radiate toward the knee. It often worsens with activity and may ease with rest in the early stages.
Morning stiffness or stiffness after sitting
The hip may feel tight or restricted, particularly after rest or when first getting up in the morning.
Reduced range of motion
Movements such as bending, rotating the leg, or tying shoelaces may become harder over time.
Limping or altered walking pattern
As the pain increases, you may find yourself unconsciously adjusting how you walk to minimise discomfort.
Clicking, grinding, or catching sensations in the joint
These may be signs that the smooth cartilage surface of the joint has worn down.
Increased discomfort with weight-bearing
Activities such as standing, walking long distances, climbing stairs, or carrying groceries may become more difficult.
Some patients are surprised to learn that arthritis in the hip can cause pain referred to other areas, including the front of the thigh or even the knee. This overlap can sometimes make diagnosis less straightforward without imaging.
If you’re noticing several of these symptoms, particularly if they’re affecting your ability to stay active, it may be a sign of underlying joint degeneration.
Are you a candidate for hip replacement surgery? Key factors Dr Hockings will consider
Total hip replacement surgery is generally recommended when the hip joint has become so damaged that it significantly affects your comfort, mobility, or ability to participate in daily life. It is not typically a first step in treatment but may be considered when non-surgical options such as physiotherapy, weight management, anti-inflammatory medications, and joint injections no longer provide enough relief.
Whether you are a suitable candidate for surgery depends on a combination of clinical findings, imaging, and how much your symptoms are impacting your everyday function.
Factors that influence surgical suitability:
- Severity of joint damage: Imaging, such as X-rays or CT scans, can show the extent of cartilage loss, narrowing of the joint space, bone spurs, or other degenerative changes. When there is bone-on-bone contact, surgery is more likely to be appropriate.
- Functional limitations: Difficulty walking, dressing, or completing household tasks often signals a level of joint deterioration that may benefit from surgical intervention. If pain affects your ability to work, care for yourself, or engage socially, these factors are also considered.
- Response to non-surgical treatment: Surgery is usually only considered when other options have not provided satisfactory relief or have become less effective over time.
- General health and lifestyle factors: Your age, weight, activity level, and any other medical conditions are taken into account when assessing risk and potential benefit. The decision is always made with your safety and recovery in mind.
- Personal goals and expectations: Some people aim to return to recreational activities or travel, while others may simply want to walk short distances without pain. Your goals help shape the treatment plan.
Hip replacement can be a highly effective procedure for the right person, but it is not suitable for everyone. The decision to proceed with surgery is made after a comprehensive assessment, with clear consideration of your individual needs and long-term outcomes.
For people with significant arthritis affecting both hips, Dr Jason Hockings may discuss the option of bilateral hip replacement. This involves replacing both hip joints, either during the same operation (simultaneous) or in two separate procedures performed months apart (staged).
A simultaneous bilateral hip replacement may be suitable for individuals who are medically fit, highly motivated for rehabilitation, and have appropriate support at home. Potential advantages can include a single hospital stay, one anaesthetic, and a unified recovery period.
In some cases, a staged approach, where one hip is replaced and the second surgery is performed after recovery from the first, may be safer and more practical. This allows one leg to support mobility, balance, and independence during early rehabilitation.
Because recovery from bilateral surgery can be more physically demanding in the initial weeks, careful assessment is essential. Dr Hockings will consider your overall health, mobility, home environment, and personal goals before recommending whether a simultaneous or staged approach is the most appropriate option for your circumstances.
Dr Hockings will take steps to minimise your surgical risk, including enhanced recovery protocols, prophylactic antibiotics, and blood clot prevention measures.
When a hip replacement might not be the right option for you
Although total hip replacement can offer significant pain relief and improved mobility, it is not appropriate for every patient. In some cases, alternative treatments may be more suitable, or surgery may need to be delayed until certain risks are addressed. Understanding when hip replacement may not be the best option is just as important as knowing when it is.
Situations where surgery may not be recommended
- Mild or early-stage arthritis: If joint damage is minimal and symptoms are manageable with non-surgical treatments, surgery is usually not advised. In these cases, physiotherapy, medications, and lifestyle changes may be effective in reducing symptoms and slowing progression.
- Active joint or systemic infection: Surgery must be postponed if there is an active infection anywhere in the body. Introducing a prosthesis into an infected environment can lead to serious complications.
- Uncontrolled medical conditions: Significant heart, lung, or kidney problems may increase the risks of surgery and anaesthesia. These issues often need to be optimised with your general practitioner or specialist team before any procedure is considered.
- Severe obesity or frailty: Excessive body weight or very low muscle strength can increase the risk of complications and slow post-operative recovery. In some cases, weight management or prehabilitation may be recommended first.
- Poor skin condition near the surgical site: Open wounds or dermatological issues over the hip area may increase infection risk and may require treatment before surgery is safe.
- Very high physical demands: If your lifestyle involves heavy manual labour or high-impact sports, the longevity of the implant may be reduced. Other joint preservation options might be discussed depending on your age and goals.
It is also important to have realistic expectations. While hip replacement can significantly reduce pain and improve function, it may not fully restore the joint to what it once was. A careful discussion about your goals, limitations, and recovery is an essential part of the decision-making process.
Total hip replacement surgical approaches and techniques
Hip replacement surgery can be performed using several different surgical approaches. The way the hip joint is accessed, known as the surgical approach, can influence muscle preservation, recovery, and the positioning of the prosthetic components. There is no single “best” technique for every patient; the most appropriate approach depends on your anatomy, joint condition, medical history, and individual recovery goals.
Dr Hockings is experienced in multiple approaches, including the anterior approach, posterior approach, and bikini incision techniques. Each method provides specific advantages in terms of exposure, soft tissue handling, and incision placement.
How the surgical approach is chosen
Before surgery, detailed imaging and planning software are used to assess your hip joint in three dimensions. The choice of surgical approach is influenced by:
- The size and shape of your pelvis and femur
- The presence of joint deformity, contractures, or previous injuries
- Your overall flexibility and muscle strength
- Any previous surgery or scarring in the area
- Your body shape and general health status
The aim is to choose a method that allows the safest access to the joint and supports a strong, stable result.
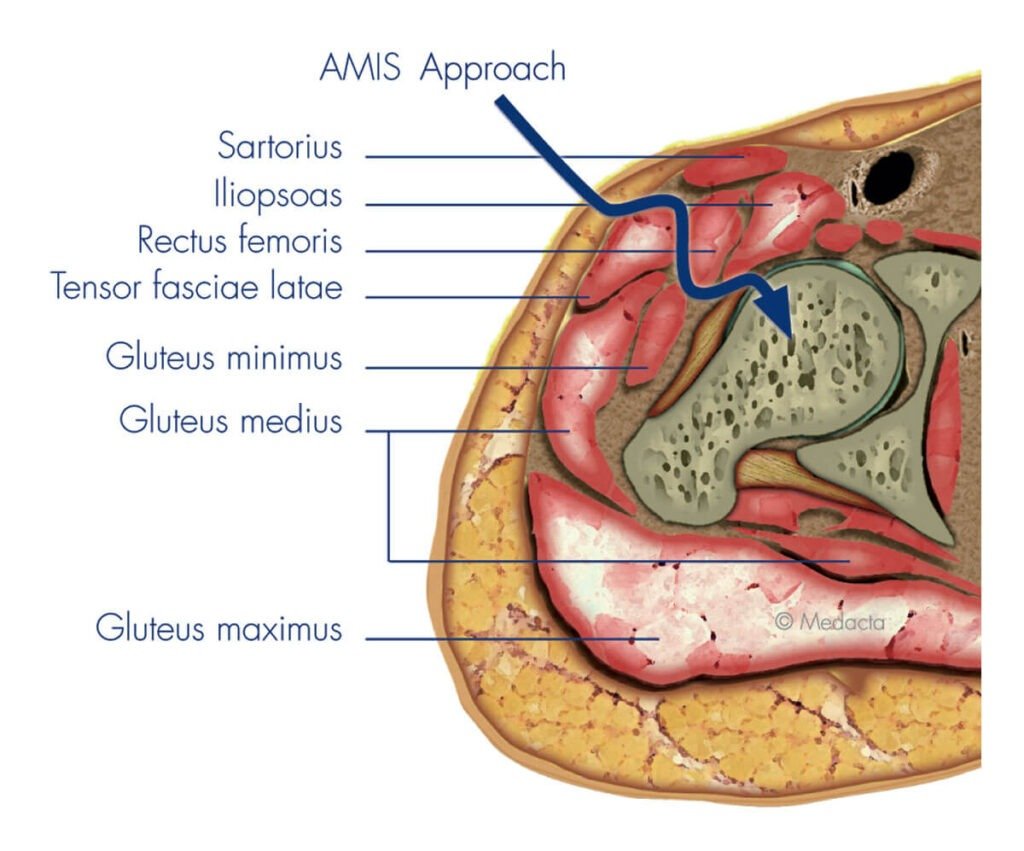
Dr Hockings frequently performs total hip replacement using the anterior approach, which allows access to the joint from the front of the hip. This technique follows a natural path between muscles rather than cutting through them, which may result in less soft tissue trauma during surgery.
Potential benefits of the anterior approach may include:
- A smaller surgical incision at the front of the hip
- Earlier mobilisation and walking after surgery
- Reduced disruption to muscles and tendons
- Lower early dislocation risk in some cases
Dr Hockings has undertaken post-fellowship training in anterior hip replacement and uses this method when it is safe and appropriate for the patient. In suitable cases, it can also be performed using a bikini incision, which follows the natural line of the groin crease.
The posterior approach: a versatile option for complex or revision cases
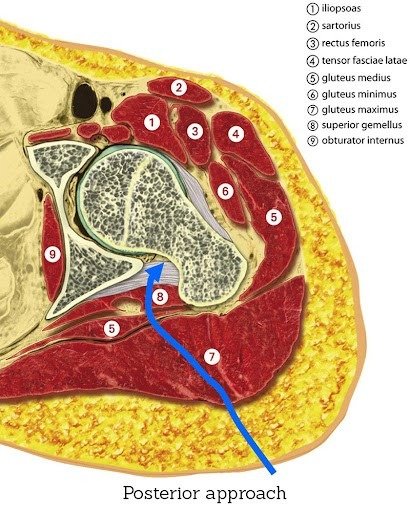
The posterior approach accesses the joint from the back of the hip and remains a well-established and widely used technique. It provides excellent visibility of the joint, which is especially useful when dealing with:
- Abnormal bone anatomy
- Significant joint deformity
- Revision procedures where old implants must be removed
- Stiffness or contractures that limit joint access
Although the posterior approach involves releasing some muscles and soft tissue, these are repaired during closure. With the right surgical technique and rehabilitation, long-term outcomes remain excellent.
Regardless of the surgical approach used, Dr Hockings focuses on achieving a stable, well-functioning joint. Careful attention is given to:
- Balancing leg lengths
- Ensuring joint stability through the full range of motion
- Minimising soft tissue trauma
- Accurately positioning each implant component
Your surgical approach will be selected as part of a personalised plan designed to support your recovery and long-term mobility.
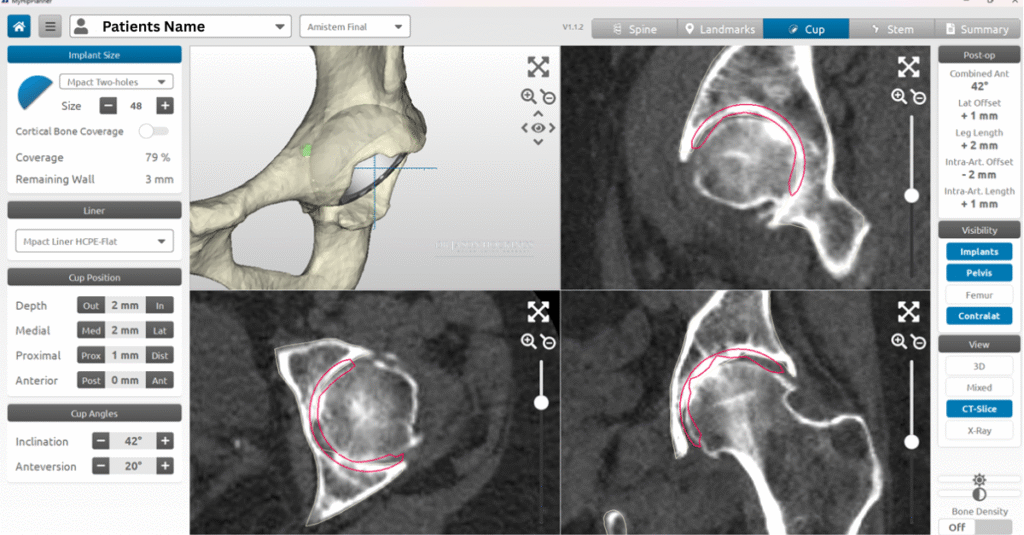
Recognising that every hip is different, Dr Hockings incorporates digital imaging and surgical planning tools to measure your anatomy before surgery, plan component sizes, and optimise placement of the implants. This means that, for suitable patients, patient-specific instrumentation (PSI) may be used to tailor the procedure to your exact bone shape and alignment.
Understanding the prosthetic implants used in your hip replacement
In hip replacement surgery, the choice of prosthetic implant plays a vital role in your long-term comfort, mobility, and surgical success. Modern hip implants are highly advanced devices designed to restore the natural movement of the hip, relieve pain, and support your return to an active lifestyle.
A total hip replacement is made up of three main prosthetic components:
FEMORAL COMPONENT
The femoral component, or stem, is the part of your hip replacement that fits inside the thigh bone (femur) to support the new joint. The specific implant selected depends on factors such as your bone quality, the shape of your femur, and your individual surgical plan.

ACETABULAR COMPONENT
The acetabular component replaces the socket of your hip joint. It usually consists of a titanium shell that fits securely into the pelvis, with a smooth inner liner made from either ceramic or highly cross-linked polyethylene to allow smooth movement of the joint.

ARTICULAR INTERFACE
The articular interface is the contact point between the femoral head (ball) and the liner within the socket. This surface allows the components to glide smoothly against each other, playing an essential role in joint movement, comfort, and the long-term performance of your hip replacement.

In most total hip replacement procedures, Dr Hockings uses the AMIStem-P Collared Femoral Component, designed to support bone preservation and long-term stability, together with the M-Pact Acetabular Cup system, which provides strong fixation and accommodates individual anatomical variation. These implants are developed by Medacta International, a Swiss orthopaedic company recognised for its evidence based approach to joint replacement innovation. While Dr Hockings frequently uses this combination, he carefully assesses each patient’s anatomy, bone quality, and surgical goals to determine the most appropriate implant configuration.
What are the potential risks of hip replacement surgery?
While total hip replacement is a common and generally safe procedure, like all surgeries, it carries certain risks. Understanding these risks can help you make an informed decision and recognise any signs that may require further attention during your recovery. Dr Hockings will discuss these potential risks with you during your consultation and take every precaution to minimise them.
Common surgical risks
Infection
This can occur in the wound or deep around the implant. Antibiotics are routinely given before and after surgery to reduce this risk.
Blood clots (deep vein thrombosis or DVT)
These can form in the leg after surgery. Preventative measures include early mobilisation, compression stockings, and blood-thinning medication.
Bleeding or haematoma
Some bleeding is normal, but occasionally a collection of blood may form around the joint, requiring further management.
Pain or stiffness
Some patients may experience persistent pain, limited range of motion, or stiffness despite a successful procedure. Rehabilitation is key to reducing these risks.
Delayed wound healing
Some wounds may take longer to heal due to factors such as diabetes, smoking, or poor circulation.
Risks specific to total hip replacement
Dislocation of the hip joint
A hip replacement relies on the surrounding muscles and soft tissues for stability. In some cases, the new joint may dislocate if the ball comes out of the socket. This risk is higher in the early weeks after surgery while the tissues are healing. You will receive guidance on movements to avoid during your recovery.
Leg length difference
Although every effort is made to match your leg lengths, some patients notice a small difference after surgery. This is often due to the need to optimise stability in the hip. If present, it may improve over time or be managed with physiotherapy or shoe inserts if needed.
Loosening or wear of the implant over time
Hip implants are designed to be durable, but they can wear down or loosen gradually. This often occurs many years after surgery. If the implant becomes worn or loose, further surgery may be required.
Nerve or blood vessel irritation
The major nerves and blood vessels around the hip are protected throughout surgery, though irritation or injury can occasionally occur. This may lead to numbness, weakness, or altered sensation, which in most cases improves gradually with time.
Fracture around the implant
Rarely, small fractures of the bone around the implant may occur during or after surgery. These are more common in people with weaker bone quality. If this happens, additional fixation or a change in rehabilitation may be required.
Reaction to bearing surfaces
Modern hip replacements use materials designed for long-term function. Very rarely, patients may develop reactions to wear particles, inflammation, or local tissue changes. Monitoring and follow-up appointments are important to detect these changes early.
Dr Hockings will take steps to minimise your surgical risk, including enhanced recovery protocols, prophylactic antibiotics, and blood clot prevention measures.
How hip replacement surgery may improve your daily comfort and mobility
The primary goal of surgery is to reduce pain and help you return to the activities you enjoy. After recovery, most patients experience:
Reduction in hip pain
Most people notice a significant decrease in hip pain once the damaged joint surfaces have been replaced. By removing the worn cartilage and arthritic bone, the procedure aims to relieve the discomfort that has been affecting your daily life.
Improved movement and flexibility
As the new prosthetic components create a smoother joint surface, you may experience better mobility and a more natural range of motion. Simple tasks such as walking, standing, and bending often become easier as healing progresses.
Greater ease with daily activities
With a more stable and functional hip joint, many individuals find it easier to perform everyday tasks such as getting dressed, climbing stairs, or moving around the home. This can lead to a noticeable improvement in day-to-day comfort and confidence.
Support for independence
Hip pain and stiffness can limit your ability to participate in activities you enjoy. After recovery, many people are able to return to a more active and independent lifestyle, with fewer restrictions on movement.
Long-lasting joint performance
Modern hip implants are designed to provide durable results. While individual outcomes vary, many prosthetic hips function well for decades, helping people maintain activity levels and long-term comfort.
Returning to physical activity
After completing rehabilitation, many patients return to low-impact recreational activities such as walking, swimming, cycling, golfing, and doubles tennis. These activities may help maintain fitness and joint strength without placing excessive load on the new hip.
A total hip replacement may offer meaningful improvements in comfort and mobility for many people living with severe hip arthritis. Dr Hockings will discuss the potential benefits and the expected recovery timeline so you can make an informed decision that feels right for your situation.
The Process
Your patient specific, total hip replacement journey with Dr Jason Hockings: step by step
If you and Dr Jason Hockings decide that total hip replacement surgery is the right option for you, it’s natural to want to understand what the process involves. This step-by-step guide outlines what to expect from your initial consultation through to surgery and recovery, using Dr Hockings’ advanced, patient-specific approach. Every aspect of your care, from pre-operative planning to rehabilitation is tailored to your individual anatomy, lifestyle, and recovery goals to help you achieve the best possible outcome.
Step 1.
GP referral and consultation

Your journey begins with a referral from your GP or another medical specialist. This referral is required to book your first appointment with Dr Jason Hockings and ensures you receive the applicable Medicare rebate.
At your initial consultation, Dr Hockings will take a detailed medical history, review any previous imaging, and perform a clinical assessment of your hip. He’ll discuss your symptoms, lifestyle goals, and the non-surgical and surgical treatment options available. This appointment is also an opportunity for you to ask questions and gain a clear understanding of the procedure, recovery process, and expected outcomes.
If total hip replacement is considered the most appropriate treatment, Dr Hockings will organise further diagnostic imaging to assist with surgical planning. You’ll be referred for a CT scan, which is used to create a 3D model of your hip using MyHip software for precise, patient-specific planning. Additional tests such as X-rays, blood tests, and general health checks may also be arranged as needed.
Once all results are reviewed, Dr Hockings will explain the surgical procedure in detail, including the potential benefits, risks, and expected recovery milestones. When you feel confident and fully informed, you’ll complete the surgical consent form. You’ll also receive personalised advice on preparing your home and arranging any support you may need during your recovery period.
Step 2.
Pre-operative surgical plan analysis
Once your CT scan has been completed, Dr Jason Hockings will use the data to develop a personalised 3D surgical plan using MyHip digital planning software. This system allows him to visualise your hip joint in three dimensions and assess your bone shape, joint orientation, and surrounding anatomy with precision.
Using this model, Dr Hockings can plan the size, position, and alignment of each implant component before surgery. This planning helps guide leg length, joint stability, and muscle balance while minimising the need for adjustments during the procedure.
Step 3.
Surgical preparation and pre-operative steps

In the weeks leading up to surgery, you’ll receive guidance and support from Dr Hockings and his team to help you prepare physically and practically for your procedure. This preparation phase is important for achieving a smooth recovery and ensuring your surgery proceeds safely.
You may also be asked to attend a pre-admission clinic or health assessment, which may include a review by your anaesthetist and the hospital nursing team. During this visit, your medical history, current medications, allergies, and recent test results will be carefully reviewed to ensure you are ready for surgery.
Dr Hockings may also provide advice on:
- Maintaining or improving your fitness and mobility before surgery.
- Reviewing medications that may affect your operation or recovery.
- Preparing your home environment, such as setting up supportive seating, removing trip hazards, or installing handrails.
- Arranging time off work and planning support from family or friends during the early stages of recovery.
You’ll also receive a pre-surgery information pack from the hospital and Dr Hockings’ team, which includes:
- Hospital admission paperwork.
- Education about fasting instructions and medication management.
- Guidance on prehabilitation physiotherapy (where appropriate).
- Information about mobility aids and home preparation.
These steps are designed to ensure you feel confident, informed, and well prepared before your operation.
Step 4.
Anaesthesia consultation
 Before your procedure, you’ll have a pre-operative consultation with the anaesthetic team, usually conducted over the phone. During this conversation, the anaesthetist will review your medical history, current medications, and any previous experiences with anaesthesia. This is an important step in ensuring your safety and comfort during surgery. Together, you’ll discuss the two main types of anaesthesia used in hip replacement surgery; spinal anaesthesia and general anaesthesia and determine which is most appropriate for you.
Before your procedure, you’ll have a pre-operative consultation with the anaesthetic team, usually conducted over the phone. During this conversation, the anaesthetist will review your medical history, current medications, and any previous experiences with anaesthesia. This is an important step in ensuring your safety and comfort during surgery. Together, you’ll discuss the two main types of anaesthesia used in hip replacement surgery; spinal anaesthesia and general anaesthesia and determine which is most appropriate for you.
The anaesthetist will explain the risks and benefits of each option and answer any questions you may have. Their goal is to create a personalised anaesthetic plan that prioritises your comfort, supports a smooth surgical experience, and promotes a safe recovery.
Step 5.
On the day of surgery
On the day of your surgery, you’ll be admitted to hospital and greeted by the nursing and anaesthetic teams, who will guide you through the pre-operative process.
Before your procedure:
- You’ll meet Dr Jason Hockings, who will review your surgical plan and confirm the procedure details.
- Your anaesthetist will discuss the type of anaesthetic (usually a spinal anaesthetic with sedation) and answer any final questions.
- The surgical site will be marked, and your hip area will be prepared in the anaesthetic bay.
- Routine checks such as identification, consent verification, and allergy review will be performed.
The operating theatre team will then escort you into theatre, where your procedure will be performed in a carefully controlled, sterile environment. Throughout the operation, your anaesthetic and surgical teams will monitor your comfort and safety closely.
Step 6.
The total hip replacement surgical procedure
Surgical incision: Once the anaesthetic has taken effect, Dr Hockings makes a small incision at the front of your hip, usually near the natural crease of the upper thigh. In selected patients, a bikini incision may be used. This involves placing the incision within the natural skin crease to improve cosmetic appearance while still allowing safe access to the hip. The length of the incision varies depending on your body shape and the surgical exposure required but is kept as small as safely possible to allow accurate placement of the components.
Accessing the hip joint: Through the incision, Dr Hockings works between the muscles rather than cutting through them. This muscle-sparing approach is one of the key features of the anterior technique and may support more comfortable early movement after surgery. The muscles and soft tissues are gently moved aside to expose the hip joint in a controlled and accurate way.
Removing the damaged hip joint: Using the personalised 3D MyHip surgical plan as a guide, Dr Hockings removes the worn surfaces of your ball-and-socket joint. This includes:
- Removing the arthritic femoral head
- Cleaning out damaged cartilage and preparing the hip socket (acetabulum)
This step is tailored to your unique anatomy to help ensure an accurate fit for the prosthetic components.
Preparing the hip socket: The acetabulum is reshaped and smoothed to create a stable foundation for the new socket component. The MyHip plan helps guide the position, angle, and depth of preparation so the implant sits securely and functions smoothly.
Trial acetabular component placement: A temporary trial cup is positioned in the prepared socket to check alignment, stability, and overall fit. This step allows fine adjustments before the final component is implanted.
Inserting the acetabular cup: Once everything is confirmed, the final cup is inserted into the socket. A liner is then placed inside the cup to create the low-friction surface that allows your new hip to rotate, bend, and move comfortably.
Preparing the femur: The femur is prepared to receive the stem component. Specialised instruments shape the canal inside the thigh bone in line with the 3D plan. A trial stem and trial head are then placed to check leg length, implant angles, soft tissue tension, and overall joint stability.
Inserting the femoral component: Once satisfied with the trial positioning, Dr Hockings inserts the final femoral stem. The design of the stem allows it to sit securely within the bone to provide long-term stability.
Attaching the femoral head: A metal or ceramic head is attached to the top of the stem. This becomes the new ball of the joint and is placed into the previously inserted socket liner, completing the reconstructed ball-and-socket structure.
Final adjustments: Before completing the surgery, Dr Hockings performs detailed checks to ensure:
- Leg length is balanced
- The joint moves smoothly
- The implant is stable throughout a full range of motion
- The components are positioned as planned using the MyHip model
These checks help support reliable function and comfort after surgery.
Closing the incision: The tissues are gently returned to their natural position, and the incision is closed with dissolvable sutures. A local anaesthetic is applied to the area to help with early pain control. Dissolvable stitches typically soften and break down gradually over several weeks.
The operation generally takes between 1 to 2 hours, although this can vary depending on your individual needs. Most patients stay in hospital for 2 to 4 days, with the exact duration tailored to your recovery progress and overall health.
This step-by-step process is designed to deliver a personalised, precise, and thoughtful surgical experience, restoring function, comfort, and quality of life through advanced hip replacement care.
Pain management after hip replacement: what you can expect
Managing your pain effectively is a key part of your recovery after hip replacement surgery. Dr Hockings and his team will implement a structured multimodal pain relief plan, aimed at reducing discomfort while minimising the use of strong opioids where possible. This approach supports early movement and helps you get back on your feet safely and confidently.
Immediately after surgery
In the hours following your procedure, managing pain and swelling is a priority. You’ll be given a combination of medications and therapies to keep your discomfort under control, allowing you to start walking with assistance as early as the same day.
Medications you may be prescribed
You’ll be given a combination of the following medications. These should be taken according to the instructions on the packet or as directed by the hospital:
- Paracetamol (e.g. Panadol Osteo): This is a core part of your pain control and should be taken regularly. It is usually the last pain reliever you stop using.
- Anti-inflammatories (e.g. Celebrex): If safe for you to take, anti-inflammatory medications help reduce both pain and swelling. Most patients use these regularly for about one week after surgery.
- Pantoprazole: If you are taking anti-inflammatories, this medication may be used to protect your stomach and reduce the risk of irritation. It can be stopped when you no longer require anti-inflammatories.
- Palexia: This is a strong pain medication that may be used regularly in the first few days. You can taper off earlier if your pain is well controlled.
- Endone: Another strong pain reliever, used only if breakthrough pain occurs and other medications are not enough. It is taken as needed.
Additional pain and swelling management strategies
- Ice therapy: Applying an ice pack (wrapped in a towel) over the hip can help reduce swelling and ease discomfort. Do not apply ice directly to the skin.
- Compression and elevation: These techniques may help limit swelling and support healing in the first few days.
- Physiotherapy: Early and gentle movement under the guidance of your physiotherapist also contributes to pain relief and helps prevent stiffness.
Expected pain timeline
- Marked improvement in walking, sitting, and sleeping
- Reduced need for strong pain medications
- Better confidence and independence in movement
- Ability to resume low-impact exercise such as cycling, swimming, and golf
Most patients find that pain steadily improves over the first 2–3 weeks after surgery. You may still experience some discomfort with activity or at night during the early stages of healing, but this typically settles with time, movement, and gradual reduction of medications.
Your recovery timeline after total hip replacement surgery
The typical recovery following total hip replacement through a direct anterior approach is often faster compared to traditional approaches. However, it’s important to note that individual recovery experiences can vary based on factors such as the patient’s overall health, preoperative fitness, and adherence to rehabilitation protocols.

Here is a general overview of the recovery process:
Immediate Postoperative Period (Days 1-3)
- Patients are encouraged to start moving and walking with assistance on the day of surgery.
- Pain management is a priority to ensure comfort during the initial recovery phase.
- Physiotherapy may begin soon after surgery to facilitate early mobilisation and teach proper movement techniques.
While you’re in hospital, a physiotherapist will get you moving safely, often on the same day or the morning after surgery. You’ll start with:
- Gentle exercises to keep the joint mobile and reduce stiffness
- Muscle activation and strengthening exercises that don’t overload the new joint
- Walking with crutches or a frame, to help you move confidently and avoid strain
Weeks 1-6
Activity Guidelines After Surgery
- Weight-bearing: Dr Hockings will advise how much weight you can place on your new hip, depending on your surgical approach and implant. Most patients begin walking with a frame or crutches on the same day or the morning after surgery.
- Gentle exercises: Start with simple movements recommended by your physiotherapist to maintain flexibility and prevent stiffness.
- Avoid high-impact movements: Running, jumping, or lifting heavy items should be avoided to protect the healing joint.
- Pace yourself: Gradually build up activity, listen to your body, and rest as needed to avoid overdoing it.
- Patients continue with physiotherapy to improve strength, flexibility, and walking abilities.
- Gradual resumption of daily activities with precautions to avoid certain movements that may stress the hip joint.
- Most patients are able to walk with a cane or walker, gradually transitioning to walking without assistance.
Weeks 6-12
- Continued improvement in mobility and strength.
- Transition to more independent daily activities, including driving (if approved by the surgeon) and light recreational activities.
- Follow-up appointments with Dr Hockings to monitor progress.
Months 3-6
- Further gains in strength and mobility.
- Patients often resume more normal activities, including low-impact exercises and recreational pursuits.
- Full recovery may take several months, and patients are advised to avoid high-impact activities.
Months 6 and Beyond
- Continued improvement in strength and endurance.
- Patients can often return to more demanding activities, including sports, under the guidance of Dr Hockings.
Physiotherapy to Support Recovery
Physiotherapy plays a vital role in your recovery after hip replacement surgery. It helps restore mobility, build strength, and guide you safely back to everyday activities. Dr Hockings works closely with physiotherapists to tailor your rehab to your needs and surgical approach.
At home or outpatient physiotherapy
Once discharged, your rehab will continue with either home visits or outpatient sessions. This phase focuses on:
- Active movement exercises to improve control and reduce tightness
- Gradual weight-bearing, depending on your progress and surgical approach
- Functional training; learning how to safely walk, climb stairs, and move in and out of bed or chairs
Later stages of recovery
As you gain strength, your physiotherapist will guide you through more advanced exercises to:
- Improve balance and endurance
- Build muscle strength and joint stability
- Prepare you to return to hobbies, light sport, and normal daily life
Working with a physiotherapist is one of the most important ways to get the best result from your surgery. Dr Hockings and his team will ensure your rehab program supports your recovery every step of the way.
Activity Guidelines After Surgery
Intermediate Recovery (6 Weeks – 6 Months)
- Continue physiotherapy: Stay consistent with your exercises to strengthen the muscles supporting your hip.
- Low-impact activities: You may start using a stationary bike, swimming (once your wound has healed), or taking longer walks.
- Transition off walking aids: With approval from Dr Hockings, begin reducing your reliance on crutches or a frame as strength and balance improve.
- Be cautious with movement: Avoid twisting, pivoting, or sudden changes in direction that could place stress on your new hip.
Ongoing Recovery (6 Months and Beyond)
- Stay active: Aim for regular exercise to keep your hip strong and flexible.
- Choose joint-friendly options: Gentle activities like walking, hydrotherapy, tai chi or yoga may be helpful, depending on your goals and mobility.
- Progressive strengthening: Incorporate strength training under guidance to support your hip—but avoid exercises that cause pain or instability.
- Regular reviews: Keep up with scheduled follow-up appointments with Dr Hockings to monitor your progress and implant health.
Making Lifestyle Adjustments
- Maintain a healthy weight: Reducing excess pressure on your hip can help your implant last longer and support overall wellbeing.
- Safe home environment: Remove trip hazards, consider using grab bars or a raised toilet seat, and make sure your living space supports easy movement.
- Supportive footwear: Choose shoes with good grip and cushioning to aid balance and reduce joint stress.
- Quit smoking: Smoking can slow wound healing and increase the risk of complications. Stopping can significantly support your recovery.
- Stay connected with your healthcare team: Following Dr Hockings’ advice and attending all check-ups ensures the best possible long-term results.
By following these recovery guidelines and making positive adjustments to your lifestyle, you’ll give yourself the best chance of enjoying a strong, active, and pain-free future after hip replacement surgery with Dr Hockings.
Post-operative care and important precautions during recovery
After your hip replacement surgery, caring for your new joint is an essential part of the healing process. While modern techniques like the anterior approach offer a lower risk of dislocation, it’s still important to follow specific precautions, especially in the first 4 to 6 weeks after surgery to protect your hip as it heals and to support a smooth recovery. The precautions you’ll need to follow may vary depending on the surgical approach used. Dr Hockings will provide you with personalised advice based on your procedure and individual needs.
General precautions for all patients
Regardless of the approach used, the following general guidelines apply to support your recovery:
- Avoid low or soft seating: Choose firm chairs with straight backs and armrests. Avoid couches or deep chairs that may cause your hip to bend too much when sitting or rising.
- Use assistive devices: Reachers, long-handled shoehorns, or dressing aids can help you dress and move safely without straining your new joint.
- Wound care: Do not submerge your wound in baths, pools, or spas until it is fully healed and you’ve received medical clearance.
- Driving: Avoid driving until Dr Hockings confirms it is safe to do so, usually 4 to 6 weeks post-op, depending on your progress and which leg was operated on.
- High-impact activities: Sports or movements that involve twisting or jarring the hip (e.g. skiing, running, or tennis) should be avoided until you’ve been given clearance.
Anterior approach: Post-operative precautions
With the anterior approach, the hip is accessed from the front, allowing muscles at the side and back of the hip to be preserved. This approach generally carries a lower risk of dislocation, but some care is still needed in the early recovery phase.
Be mindful of the following precautions in the first 4–6 weeks after surgery:
- Avoid stepping too far backwards: Try not to extend your leg behind you or lie on your stomach. Overextending the hip can place strain on the front of the joint.
- Keep your leg aligned: Avoid turning your toes or knee outward excessively. When standing or walking, keep your feet and knees pointing forward.
- Take care with reverse movements: Use caution when stepping backwards or reaching behind you, as these actions can stress healing tissues.
Posterior approach: Post-operative precautions
If your surgery was performed using a posterior approach, the hip joint was accessed from the back, which requires more protection of the posterior structures during healing.
Be mindful of the following precautions in the first 4–6 weeks after surgery:
- Avoid twisting at the waist: Keep your hips and shoulders aligned. When turning, pivot your whole body instead of twisting from the waist.
- Limit bending at the hip: Do not bend forward past 90 degrees, such as when sitting low, tying shoes, or picking up items. Use tools or ask for assistance.
- Do not cross your legs or ankles: Keep both legs aligned and your feet flat when sitting or lying down to reduce strain on the hip.
Balancing movement and rest
As you recover, it’s important to steadily increase your activity level, while also listening to your body and allowing time to rest. Your physiotherapist will guide you through safe exercises to rebuild strength and confidence in your new hip.
Adjusting your lifestyle after hip replacement: returning to the activities you enjoy
Recovering from total hip replacement is the beginning of a new chapter, one where many people experience improved mobility, greater independence, and reduced discomfort. While Dr Hockings provides the surgical foundation, your commitment to safe movement and regular exercise plays an important role in long-term success.
As your strength improves, low-impact activities such as walking, swimming, cycling, and using an exercise bike are often encouraged. When your physiotherapy team feels it is appropriate, you may also be able to return to recreational activities like golf and doubles tennis, which allow you to stay active without placing excessive load on the new hip.
It is important to reintroduce activities gradually and follow the guidance provided by Dr Hockings and your physiotherapist. Listening to your body, pacing your progress, and maintaining regular movement can support the long-term function of your hip replacement and help you return to the activities you enjoy.
Hip replacement surgery FAQs
How long does a hip replacement last?
Modern hip implants can last 15–20 years or more. Implant longevity depends on your age, activity level, and how well the joint is looked after.
Will I need another surgery in the future?
Younger, more active patients may eventually require a revision hip replacement. Dr Hockings selects implants with a strong long-term track record to help delay or reduce the need for future surgery.
Can both hips be replaced at once?
Yes, in some cases. Learn more about Bilateral Hip Replacement
Is anterior approach hip replacement better?
It may allow for quicker early recovery in some patients, but it’s not suitable for everyone. Dr Hockings will assess and explain your options. Learn more about Anterior Approach Hip Replacement Surgery

If you’re experiencing ongoing pain, stiffness, or reduced movement that is affecting your daily activities or quality of life, a thorough orthopaedic assessment can help determine the cause and guide the most appropriate treatment options for your situation.