- SPECIALIST ORTHOPAEDIC SURGEON | MELBOURNE, VIC | ALBURY, NSW | MORNINGTON, VIC |
- 03 9421 6133
Shoulder Arthritis
Understanding pain, stiffness, and joint degeneration in the shoulder
Shoulder arthritis refers to the gradual wearing down of the cartilage that lines the ball-and-socket joint of the shoulder. As this protective cartilage deteriorates, the bones of the joint begin to rub against each other, leading to pain, stiffness, swelling, and reduced function. Over time, the condition can significantly interfere with daily activities, such as reaching overhead, lifting, dressing, or sleeping comfortably.
There are several types of arthritis that can affect the shoulder, but the two most common are:
- Osteoarthritis: also known as “wear-and-tear” arthritis, this degenerative condition develops gradually with age or repetitive use.
- Rotator cuff tear arthropathy : a specific form of arthritis that occurs after a long-standing rotator cuff tendon tear, which alters shoulder mechanics and leads to joint damage.

Less commonly, shoulder arthritis may result from previous trauma (post-traumatic arthritis), inflammatory conditions (such as rheumatoid arthritis), or avascular necrosis (loss of blood supply to the bone).
Dr Jason Hockings provides comprehensive assessment and tailored treatment options for shoulder arthritis, with a focus on preserving function, relieving pain, and improving your quality of life. Whether through non-operative care or joint replacement surgery, treatment is personalised to your condition, goals, and activity level.
Common Symptoms of Shoulder Arthritis?
Patients with shoulder arthritis may experience:
- Persistent, dull or aching pain in the shoulder joint
- Pain that worsens with movement or activity
- Night pain or difficulty sleeping on the affected side
- Stiffness and reduced range of motion
- Grinding, clicking, or catching sensations
- Weakness when lifting or reaching overhead
- Difficulty with everyday tasks such as grooming, dressing, or putting on a seatbelt
These symptoms tend to worsen gradually over time. In some cases, a sudden increase in pain or loss of motion may occur if there is a progression of the underlying disease, or in cases of cuff tear arthropathy.
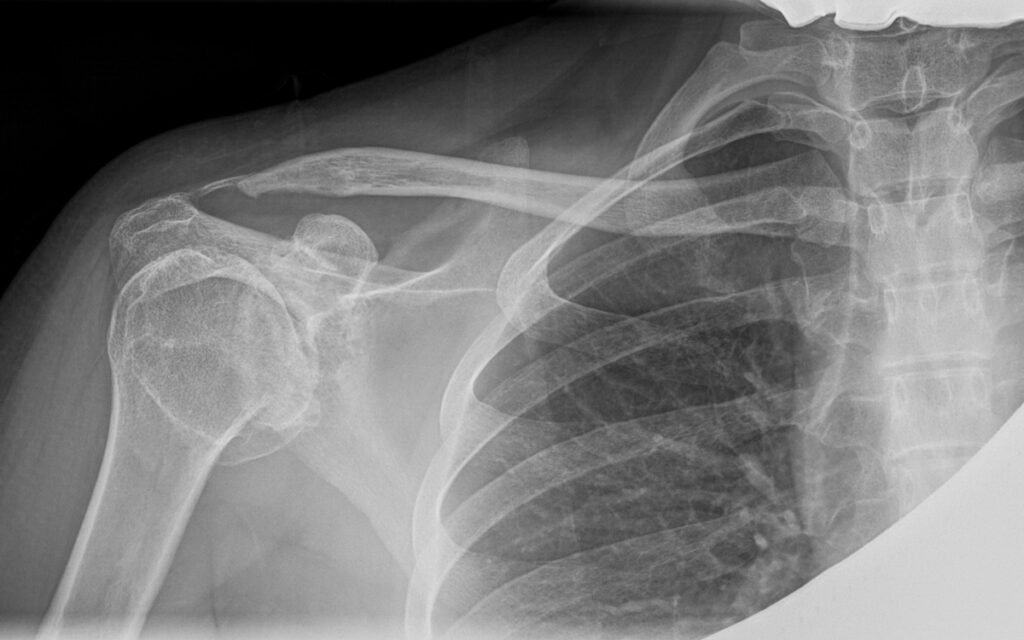
Diagnosis and imaging
A thorough clinical assessment is essential to determine the extent and cause of your shoulder symptoms. Dr Hockings will:
- Take a detailed medical history and symptom timeline
- Assess your shoulder’s range of motion, strength, and stability
- Check for signs of rotator cuff dysfunction or other underlying causes
Imaging plays a key role in confirming the diagnosis and guiding treatment decisions. Common investigations include:
- X-rays to assess joint space narrowing, bone spurs, and deformity
- Ultrasound to evaluate the rotator cuff tendons
- MRI to detect soft tissue injury, cartilage loss, or avascular necrosis
- CT scan in advanced cases or for pre-surgical planning
These tools help Dr Hockings understand the severity of arthritis, involvement of the rotator cuff, and suitability for surgical or non-surgical care.
Non-surgical management of shoulder arthritis
Not all cases of shoulder arthritis require surgery. In early or moderate stages, non-operative treatments may effectively relieve symptoms and support joint function. These may include:
- Activity modification to avoid aggravating movements
- Anti-inflammatory medications to reduce pain and swelling
- Physiotherapy focused on improving range of motion, posture, and muscle support
- Heat or ice therapy for pain control
- Corticosteroid injections to reduce inflammation and improve mobility
- Platelet-rich plasma (PRP) or other biologic injections (select cases)
These treatments may help delay the need for surgery and improve quality of life. Dr Hockings will work with you to develop a conservative management plan tailored to your symptoms and goals.
Surgical options for shoulder arthritis
When non-surgical care no longer provides relief, surgery may be considered to restore function and relieve pain. The most common surgical procedures include:
-
Anatomical total shoulder replacement
Suitable for patients with intact rotator cuff tendons. The procedure involves replacing the damaged joint surfaces with a metal ball and plastic socket to restore smooth movement and reduce pain. -
Reverse total shoulder replacement
Often recommended when arthritis is combined with a torn or non-functioning rotator cuff. The position of the ball and socket is reversed, allowing the deltoid muscle to compensate for the damaged rotator cuff. -
Hemiarthroplasty
Involves replacing only the ball (humeral head) of the joint. This may be used in select cases, such as avascular necrosis or post-fracture arthritis. -
Arthroscopic debridement
A minimally invasive procedure used to clean out loose cartilage, bone spurs, or inflamed tissue in mild to moderate arthritis. This may offer short-term relief in early cases.
Dr Hockings will explain your options, discuss expected outcomes, and help you make an informed decision about the best course of action for your individual condition.

If you’re experiencing ongoing pain, stiffness, or reduced movement that is affecting your daily activities or quality of life, a thorough orthopaedic assessment can help determine the cause and guide the most appropriate treatment options for your situation.
