- SPECIALIST ORTHOPAEDIC SURGEON | MELBOURNE, VIC | ALBURY, NSW | MORNINGTON, VIC |
- 03 9421 6133
Shoulder instability or dislocation
Understanding shoulder looseness, partial slipping, or full dislocation
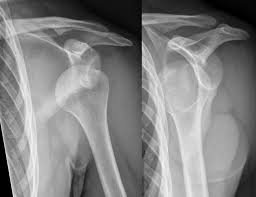
Shoulder instability occurs when the structures that support your shoulder joint, including the labrum, ligaments, and surrounding muscles become weakened, stretched, or torn. This can result in the ball of the shoulder (humeral head) moving excessively within its socket (glenoid), causing a sensation of looseness, slipping, or, in more severe cases, a full dislocation.
Shoulder dislocation happens when the ball completely comes out of the socket, usually following trauma. Some people may go on to develop chronic instability, where the shoulder repeatedly subluxes (partially slips out) or dislocates with certain movements or during sports.
Shoulder instability is more common in younger individuals and athletes involved in overhead or contact sports, such as football, basketball, swimming, or gymnastics. It may also occur with generalised joint laxity (hypermobility) or as a result of repetitive overhead strain over time.
In this section, you’ll learn about the causes and types of shoulder instability, common symptoms, how it is diagnosed, and the various treatment options, including stabilisation surgery when needed.

What causes shoulder instability or dislocation?
Shoulder instability can result from:
- Traumatic injury: A fall, sporting accident, or high-impact trauma can force the shoulder out of the socket, stretching or tearing the labrum and ligaments.
- Repetitive strain: Overhead sports such as swimming, tennis, or volleyball can gradually weaken shoulder stability through repetitive motion and microtrauma.
- Structural or anatomical factors: Some individuals have naturally looser joints (generalised hypermobility), making them more prone to instability.
- Previous dislocations: A history of dislocation increases the likelihood of future episodes, especially in younger, active individuals.
Types of shoulder instability
Shoulder instability is classified based on how it occurs and the direction of movement:
- Traumatic anterior instability – The most common type, where the shoulder dislocates forward, often after a fall or tackle.
- Atraumatic (non-injury) instability – Occurs gradually due to generalised joint laxity or repetitive overhead movement.
- Multidirectional instability – The shoulder may feel unstable in multiple directions (e.g. forwards and downwards) and is often linked to hypermobility.
- Posterior instability – Less common, usually resulting from seizures, electric shocks, or heavy lifting.
Common symptoms of shoulder instability
People with shoulder instability may experience:
- A sensation of the shoulder feeling loose, unstable, or "slipping out"
- Pain during overhead or throwing movements
- Recurrent dislocations or subluxations (partial dislocations)
- Clicking, catching, or weakness in the shoulder
- Limited function or fear of certain movements due to instability
For some, symptoms may be subtle and episodic, while others may experience frequent dislocations that interfere with sport or daily life.
How is shoulder instability diagnosed?
Diagnosis involves a thorough history, clinical examination, and imaging studies. Dr Hockings will:
- Discuss your symptoms, past injuries, and activity level
- Perform physical tests to assess stability, strength, and joint laxity
- Order imaging, such as:
- X-rays – to assess joint alignment and rule out fractures
- MRI or MR arthrogram – to evaluate soft tissue structures like the labrum, ligaments, and joint capsule
Accurate diagnosis is essential to determine the best treatment approach and prevent further damage.
Non-surgical treatment options
Not all shoulder instability requires surgery. Conservative treatment may be effective, particularly for first-time dislocations or mild instability. Non-surgical options include:
- Physiotherapy – A structured strengthening program to improve dynamic shoulder stability, especially targeting the rotator cuff and scapular muscles.
- Activity modification – Avoiding high-risk positions or movements that provoke symptoms.
- Bracing – Occasionally used in sports settings to reduce the risk of repeat dislocation.
- Pain relief – Anti-inflammatory medications or guided corticosteroid injections for associated bursitis or inflammation.
Dr Hockings will guide you through an individualised non-operative management plan where appropriate.
When might surgery be required?
Surgical intervention may be recommended if:
- You’ve experienced recurrent dislocations or subluxations
- There is confirmed structural damage to the labrum or ligaments
- You are a young, active individual at high risk of recurrence (e.g. contact athletes)
- Imaging reveals a Bankart lesion (labral tear) or bony damage such as a Hill-Sachs lesion or glenoid bone loss
Early surgical repair in certain high-risk groups may reduce the risk of future instability and help preserve joint health.
What does shoulder stabilisation surgery involve?
Shoulder stabilisation aims to restore joint stability by repairing or reconstructing the damaged soft tissue structures that keep the shoulder in place.
Dr Jason Hockings typically performs arthroscopic shoulder stabilisation, a minimally invasive procedure using small incisions and a camera-guided instrument (arthroscope).
During surgery, he may:
- Reattach torn labrum tissue to the rim of the socket using suture anchors (Bankart repair)
- Tighten or reinforce stretched ligaments or capsule (capsular shift or plication)
- Address associated conditions such as biceps tendon injury or rotator cuff tears
In more complex cases, open procedures or bone block techniques (e.g. Latarjet) may be considered, particularly when bone loss is present.
You’ll wear a sling for several weeks to protect the repair. Physiotherapy begins gradually with passive movements, followed by active strengthening from 6–12 weeks. Return to contact sport is typically delayed for 4–6 months, depending on your progress.
As with any surgery, there are risks such as infection, stiffness, nerve injury, or recurrence of instability. Dr Hockings will discuss these with you during your consultation.

If you’re experiencing ongoing pain, stiffness, or reduced movement that is affecting your daily activities or quality of life, a thorough orthopaedic assessment can help determine the cause and guide the most appropriate treatment options for your situation.
