- SPECIALIST ORTHOPAEDIC SURGEON | MELBOURNE, VIC | ALBURY, NSW | MORNINGTON, VIC |
- 03 9421 6133
Reverse Shoulder Replacement
Restoring shoulder function when traditional (anatomic) replacement isn’t suitable
Reverse shoulder replacement, also known as reverse total shoulder arthroplasty (RTSA) is a specialised type of joint replacement surgery used to treat complex shoulder conditions. It is most commonly recommended when there is severe or irreparable rotator cuff damage, rotator cuff arthropathy (a combination of arthritis and cuff tearing), or a previously failed shoulder surgery.
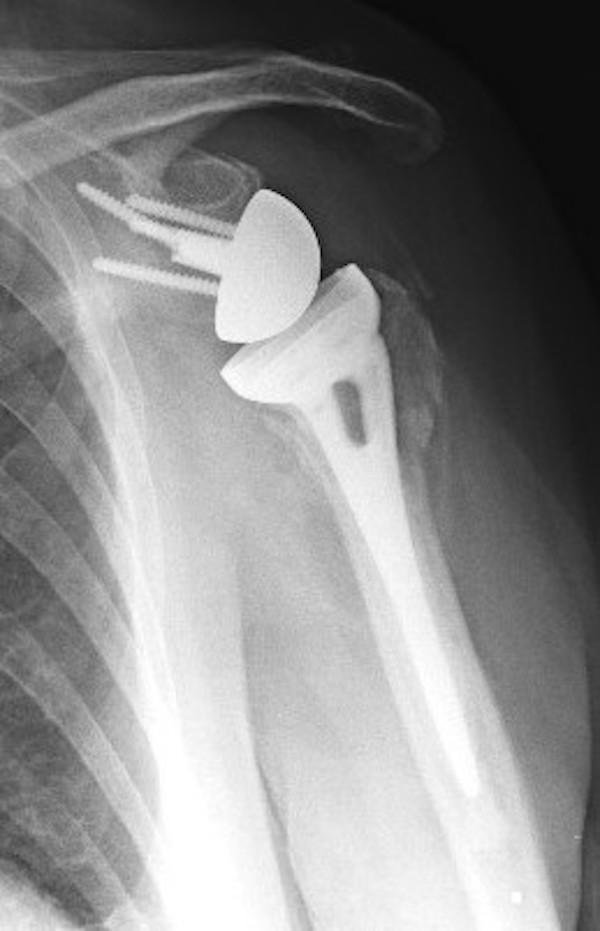
The procedure is called a “reverse” because it changes the position of the joint components: the ball-shaped implant is placed where the shoulder socket (glenoid) once was, and the socket is positioned where the humeral head used to be. This reversed design shifts the mechanics of the shoulder, allowing the deltoid muscle to take over much of the work normally done by the rotator cuff. By relying on the deltoid instead of the torn rotator cuff, reverse shoulder replacement may help restore shoulder movement, improve stability, and significantly reduce pain in patients who are no longer candidates for conventional anatomical replacement.
The information here is designed to help you understand everything involved in reverse shoulder replacement surgery, including symptoms to look out for, how the procedure works, what recovery involves, and how Dr Jason Hockings personalises care based on your needs.
Common signs and symptoms of rotator cuff arthropathy or severe shoulder damage
Rotator cuff arthropathy and complex shoulder degeneration often develop gradually, with symptoms that may be mistaken for general ageing or minor injury. Over time, damage to the rotator cuff and surrounding joint structures can significantly affect shoulder function and quality of life.
Some signs and symptoms to be aware of include:
- Ongoing shoulder pain, particularly at night or when lying on the affected side
- Difficulty lifting the arm, reaching overhead, or performing everyday tasks like brushing hair or dressing
- Weakness, especially during lifting or rotating movements
- Grinding, catching, or a feeling of instability in the shoulder joint
- Loss of shoulder motion or stiffness
- Noticeable decline in function after previous shoulder surgery
If these symptoms persist or worsen, especially in the context of a known rotator cuff tear, arthritis, or prior shoulder intervention, it may indicate more advanced shoulder joint damage requiring specialist assessment.
Are you a candidate for reverse total shoulder replacement surgery?
The primary reason to consider a reverse shoulder replacement is to relieve ongoing pain caused by supporting muscles and tendons no longer functioning effectively. Dr Hockings may discuss reverse shoulder replacement with you if you are experiencing severe shoulder pain, weakness, or loss of motion due to:
- Rotator cuff arthropathy; a type of shoulder arthritis caused by long-standing rotator cuff tears
- Massive, irreparable rotator cuff tears
- Shoulder fractures that are not amenable to repair (often in older patients)
- Failed previous shoulder replacement or surgeries
- Chronic shoulder instability or pseudoparalysis (inability to lift the arm despite an intact nerve supply)
It is typically considered when non-surgical treatments such as physiotherapy or injections have not provided adequate relief, and other surgical options are not appropriate and patients who are most likely to benefit are typically aged over 65, although younger individuals with complex shoulder conditions may also be considered.
When a reverse shoulder replacement might not be the right option for you
This procedure may not be recommended if:
- You still have an intact, functional rotator cuff and could benefit from a different surgical option (e.g. anatomical shoulder replacement or rotator cuff repair)
- You have a severe or uncontrolled shoulder infection
- There is significant nerve damage that may impair recovery
- Bone quality or soft tissue support is inadequate for implant fixation
In such cases, Dr Hockings will discuss alternative treatments tailored to your situation.
The surgical approach Dr Hockings uses for Reverse Shoulder Replacement
Dr Hockings performs reverse shoulder procedures using either a deltopectoral or superior approach, depending on your anatomy and clinical needs. During surgery, he also incorporates an augmented reality surgical platform called NextAR that uses smart glasses to provide live visual feedback based on your personalised anatomical plan.

NextAR Shoulder enhances accuracy by overlaying live metrics such as:
- Glenoid inclination and version
- Baseplate positioning and screw trajectory
- Offset and depth measurements in real time
A recent study showed exceptional alignment accuracy, with deviations from the pre-op plan as low as ~0.6° in angle and less than 1 mm in position, demonstrating superior execution of the surgical plan.
How personalised imaging and surgical planning guide your shoulder replacement
Before surgery, a CT scan is used to build a precise 3D virtual model of your shoulder. Dr Hockings uses a MyShoulder™ preoperative planning platform to simulate implant position, size, alignment, and biomechanics tailored to your anatomy.
This planning helps to reduce variability, improve surgical outcomes, and support the longevity of the implant.
The prosthetic implants used in reverse shoulder replacement surgery
Reverse shoulder replacement implants are specifically designed to change the way your shoulder functions, particularly when the rotator cuff is no longer working effectively. In this type of surgery, the traditional ball-and-socket structure is reversed:
GLENOSPHERE (BALL)
The glenosphere replaces the ball of the shoulder joint, but unlike a traditional shoulder replacement, it is fixed to the shoulder blade rather than the upper arm. It attaches securely to a metal baseplate that is anchored to the glenoid using screws. The rounded metal design creates the new “ball” of the joint and shifts the centre of rotation, allowing the deltoid muscle to raise the arm even when the rotator cuff is not functioning. Different glenosphere sizes can be selected to match the patient’s anatomy and support joint stability and mobility.

HUMERAL CUP (SOCKET)
The humeral cup replaces the socket part of the joint. It is a smooth, concave liner, often made from durable polyethylene, and is designed to articulate with the metal glenosphere. The cup provides a stable surface for controlled, balanced movement and allows the deltoid muscle to power the joint. Variations in cup depth, shape, and angulation enable the surgeon to fine-tune joint tension and movement, helping to maintain stability during everyday activities such as lifting and reaching.

HUMERAL STEM
The humeral stem sits inside the upper arm bone and forms the foundation for the humeral cup. It is typically made from strong, biocompatible metal, and may be inserted with or without cement depending on bone quality. The stem supports the prosthesis, distributes load through the arm bone, and helps maintain alignment during shoulder movement. Different stem lengths and designs allow the implant to be matched to the patient’s anatomy, contributing to the long-term stability of the overall construct.

When the components of a reverse shoulder replacement are assembled, they work together to shift the centre of rotation, giving the deltoid muscle improved leverage to lift and control the arm. This design enhances stability when the rotator cuff is no longer functioning and allows the joint to move through a more efficient biomechanical pathway. As a result, many people can regain practical movement for everyday tasks such as reaching, lifting the arm, and dressing.
This reversed configuration is especially valuable for individuals with massive rotator cuff tears, cuff tear arthropathy, complex shoulder fractures, or previous unsuccessful shoulder surgery. Modern implant systems also provide intraoperative flexibility, meaning that if a surgeon needs to convert from an anatomic to a reverse configuration (either during the initial procedure or a future revision), certain components may be retained rather than fully replaced. This can support a smoother operation and helps preserve as much natural bone and soft tissue as possible.
What are the potential risks of reverse shoulder replacement surgery?
As with any major surgery, there are potential risks, although complications are relatively uncommon. These may include:
- Infection
- Dislocation of the implant
- Fracture around the implant
- Loosening or wear over time
- Nerve or blood vessel injury (rare)
- Stiffness or reduced range of motion
Dr Hockings will discuss these risks with you and how they may apply to your individual health and surgical history.
The Process
Your reverse total shoulder replacement journey with Dr Jason Hockings: step by step
This step-by-step guide outlines what to expect from your initial consultation through to surgery and recovery, using Dr Hockings’ structured and individualised approach. Every stage of your care, from pre-operative planning to rehabilitation, is tailored to your shoulder anatomy, functional needs, and recovery goals to support the safest and most effective outcome for your situation.
Step 1.
GP referral and consultation

Your journey begins with a referral from your GP or another medical specialist. This referral is required to book your first appointment with Dr Jason Hockings and ensures you receive the appropriate Medicare rebate.
During your initial consultation, Dr Hockings will take a detailed history and perform a comprehensive shoulder examination to understand how your symptoms affect movement, strength, and daily activities. Imaging such as X-rays, ultrasound, or MRI may be reviewed or arranged to assess the condition of your shoulder joint, the rotator cuff, bone quality, and overall anatomy.
This appointment is also your opportunity to ask questions and gain a clear understanding of the condition affecting your shoulder. If reverse total shoulder replacement is recommended, Dr Hockings will explain why this option is suitable, outline the potential risks and benefits, and discuss the expected recovery pathway.
If you proceed with surgery, you will complete a consent form and receive guidance on preparing your home and organising any support you may need after the procedure. Additional assessments or investigations may also be arranged to ensure you are medically ready for surgery.
Step 2.
Pre-operative planning and surgical assessment

Once reverse total shoulder replacement has been recommended, Dr Jason Hockings will begin a detailed pre-operative planning process to ensure the procedure is tailored to your individual anatomy and shoulder function.
You may undergo additional X-rays, CT scans, or MRI to provide precise information about the condition of the shoulder joint, the extent of rotator cuff damage, and the shape and quality of the bone. These images help guide decisions about implant selection, component positioning, and whether any additional soft-tissue or bone procedures may be required.
During this stage, Dr Hockings will review your medical history, current medications, and any underlying health conditions that may influence your surgery or recovery. You may also be referred for routine blood tests or a pre-admission assessment to ensure you are medically prepared for the operation.
This planning phase is also a chance to discuss your goals, expected functional improvements, and any concerns you may have. Dr Hockings will outline the steps of the procedure in simple terms, explain the potential risks and limitations, and ensure you have a clear understanding of what to expect before, during, and after surgery.
Step 3.
Surgical preparation and pre-operative instructions

In the weeks leading up to your surgery, Dr Jason Hockings and his team will guide you through several important steps to ensure you are well prepared. You will attend a pre-admission assessment at the hospital, where your medical history, medications, allergies, and recent test results will be reviewed by the nursing and anaesthetic team. This helps ensure your surgery is performed as safely as possible.
You may receive advice from Dr Hockings regarding:
Medications that need to be paused or adjusted before surgery
Maintaining general fitness and shoulder mobility where possible
Preparing your home environment to support early recovery (for example, keeping frequently used items within easy reach or arranging help with daily tasks)
Organising support from family or friends for the first few weeks after surgery
The hospital will provide clear fasting instructions, explain when to arrive on the day of surgery, and outline what to bring with you. If required, you may also have consultations with your anaesthetist, especially if you have other health conditions that need careful management.
Some patients benefit from prehabilitation, such as gentle exercises or physiotherapy to optimise shoulder and upper-body strength before surgery. Dr Hockings will advise you if this is appropriate for your situation.
This preparation phase helps ensure you feel informed, supported, and ready for the operation, with a clear understanding of what to expect in the days leading up to your hospital admission.
Step 4.
Anaesthesia consultation

In the lead-up to your surgery, you will meet with an anaesthetist, either at your pre-admission appointment or on the day of your procedure. This consultation ensures you are medically prepared for anaesthesia and understand how your comfort and safety will be managed throughout the operation. The anaesthetist will review your medical history, any previous experiences with anaesthesia, your current medications, and any allergies or health conditions that may influence your anaesthetic plan. They will explain the recommended approach for your surgery, which may involve a general anaesthetic, a regional nerve block, or a combination of both, and will outline how pain will be controlled in the hours following surgery. For many patients, a nerve block is used to help support early comfort by temporarily reducing sensation around the shoulder.
You will also receive clear instructions about fasting, medication timing, and what to expect when you arrive at the hospital. This consultation is an important opportunity to ask questions and discuss any concerns, helping you feel informed and reassured ahead of your reverse shoulder replacement.
Step 5.
On the day of surgery
When you arrive at the hospital on the day of your procedure, the nursing team will guide you through the admission process, confirm your details, and ensure all pre-operative steps have been completed. You will change into hospital clothing, have your vital signs checked, and meet members of the surgical and anaesthetic teams. Dr Hockings will review your shoulder, confirm the surgical plan, and answer any final questions before you proceed to theatre.
In the operating suite, the anaesthetist will administer your anaesthetic, which is typically a general anaesthetic and may be combined with a regional nerve block to help support comfort after surgery. Once you are comfortable and fully prepared, you will be positioned safely for the operation, and the shoulder area will be cleaned and prepared in a sterile manner.
Every part of this process is designed to ensure your safety, comfort, and confidence as you move into surgery for your reverse total shoulder replacement.
Step 6.
The reverse total shoulder replacement surgical procedure
Reverse shoulder replacement is performed under general anaesthesia, often combined with a regional nerve block to support post-operative comfort. The procedure usually takes around 1.5 to 2 hours.
Dr Hockings begins by removing the damaged joint surfaces and preparing both the glenoid and humerus with precision. The prosthetic components are then inserted in a reversed configuration, where the ball is placed on the shoulder blade and the socket is positioned on the upper arm bone. This design allows the deltoid muscle to take over the work of a deficient rotator cuff.
Dr Hockings uses advanced implant systems and digital planning tools to support accuracy and implant positioning. In most cases, the surgery is performed through a muscle-preserving approach to help protect soft tissues and support recovery.
Most patients stay in hospital for one to two nights, depending on comfort, mobility, and overall health.
Early care focuses on pain control, joint protection, and gentle movement. You can expect your arm to be supported in a sling, with the physiotherapy team guiding safe passive exercises to prevent stiffness. Pain management will be tailored to your needs using medications and, in some cases, continued nerve block support.
Recovery timeline at a glance
Weeks 0–6: Sling for support; passive physiotherapy begins
Weeks 6–12: Gradual introduction of active movement and light strengthening
3–6 months: Steady improvement in strength, comfort, and everyday function
6+ months: Return to light recreational activities; ongoing rehab for higher-demand tasks
Dr Hockings will review your progress at scheduled appointments and coordinate your rehabilitation alongside your physiotherapist. Recovery is gradual, and while experiences vary, many people notice meaningful improvements in pain and arm function over the months following surgery.
This step-by-step process is designed to deliver a personalised, precise, and thoughtful surgical experience, restoring function, comfort, and quality of life through advanced shoulder replacement care.
Pain management after shoulder replacement: what you can expect
Dr Hockings works closely with anaesthetists and your hospital care team to ensure you are as comfortable as possible. Pain relief methods may include:
- Regional nerve blocks during surgery
- Oral pain medications
- Ice therapy and elevation
Pain generally improves significantly within the first 2–3 weeks. Long-term discomfort is often greatly reduced compared to pre-surgery levels.
Your recovery timeline after reverse shoulder replacement surgery
Recovery after reverse shoulder replacement is a structured and gradual process that allows your shoulder to heal safely while regaining function and comfort. While individual timelines may vary, most patients progress through the following phases:
Weeks 0–6: Early protection and passive movement
- Your arm will be supported in a sling at all times, except during supervised physiotherapy sessions or personal care.
- Passive range-of-motion exercises begin under the guidance of your physiotherapist to maintain joint flexibility and prevent stiffness, without straining the surgical repair.
- You should avoid lifting anything heavier than 1–2kg and restrict movements that combine extension with external rotation, as these can place stress on the new joint.
Weeks 6–12: Transition to active movement
- You will begin gentle active movements of the arm without assistance.
- Physiotherapy will gradually introduce exercises to restore mobility and coordination.
- Sling use is typically phased out during this time, depending on your progress and comfort.
3–6 months: Strengthening and functional recovery
- Focus shifts to strengthening the deltoid and surrounding shoulder muscles, which now play a greater role in shoulder function.
- You can expect to resume most low-impact daily activities, such as household tasks, dressing, and light cooking.
- With improved strength and control, many patients return to driving around 6–8 weeks after surgery, provided they have adequate range of motion and are no longer reliant on strong pain medications.
6 months and beyond: Long-term outcomes and activity return
- Range of motion, strength, and shoulder endurance continue to improve well into the second half of the year
- Recreational activities like swimming, golf, gardening, and travel are often resumed between 3–6 months, with some modifications depending on your shoulder function.
- High-demand or overhead sports may not be advised, particularly if your surgery was performed due to massive cuff damage or instability, but many patients return to active, fulfilling lifestyles with minimal long-term restrictions.
Supporting your recovery: Tailored physiotherapy and ongoing care
Your recovery is supported by a personalised rehabilitation plan, created in collaboration with trusted physiotherapists experienced in shoulder reconstruction. This program is designed to:
- Restore safe shoulder movement
- Rebuild deltoid strength and muscular control
- Improve posture, joint alignment, and shoulder mechanics
- Help you regain confidence and independence in daily life
Throughout your recovery, Dr Hockings will monitor your progress through scheduled follow-up appointments. These reviews allow him to assess healing, adjust your activity restrictions, and address any concerns early. With the right support and commitment to your rehabilitation plan, reverse shoulder replacement can significantly improve shoulder comfort, stability, and functional ability, especially when previous treatment options have not succeeded.
Returning to work, sport, and daily life after shoulder replacement
Regaining independence and returning to your usual activities are key goals following shoulder replacement surgery. Your ability to resume work, sport, and daily tasks will depend on your individual recovery progress, the type of shoulder replacement performed (reverse or anatomical), and the physical demands of your lifestyle or occupation.
Returning to work
When you can return to work will largely depend on the nature of your job:
- Sedentary or desk-based work: Most patients are able to return to light office duties within 4 to 6 weeks, once sling use has been reduced and basic shoulder movement is restored. Driving must also be safely resumed before returning to work that requires commuting.
- Light manual work: Jobs involving light lifting or repetitive arm movements may require a delay of 8 to 12 weeks, depending on your comfort and strength.
- Heavy manual labour or overhead tasks: For occupations that involve lifting, pushing, pulling, or working above shoulder height (e.g. construction, warehouse, trades), return may take 4 to 6 months or longer. These roles may require a tailored return-to-work plan and ongoing rehabilitation.
Dr Hockings will work with you and, if appropriate, your employer or occupational physician to guide a safe and staged return to work based on your functional capacity.
Returning to daily activities
Many patients find that everyday tasks become easier and less painful within 6 to 8 weeks of surgery. You may begin to resume
- Self-care tasks (dressing, grooming, cooking) by 3 to 6 weeks
- Light household activities (laundry, shopping, washing dishes) by 6 to 8 weeks
- Driving once you can safely control the steering wheel with both hands — typically around 6–8 weeks, depending on your range of motion, comfort, and whether you are off strong pain medications
During this time, your physiotherapy program will support shoulder coordination, muscle activation, and joint protection techniques to help you regain confidence and independence.
Returning to sport and recreation
Most people return to recreational activities gradually from 3 to 6 months post-surgery. Activities that do not involve high loads on the shoulder joint or forceful overhead movement are typically encouraged once strength and mobility allow. These may include:
- Walking and light cardio (stationary bike) from early recovery
- Swimming (gentle freestyle or breaststroke) after 3 months
- Golf and social tennis from 4–6 months, depending on your technique and joint control
- Gardening, light DIY, and travel typically resume between 3–6 months
Activities to avoid or modify
Certain high-impact or high-risk activities may need to be permanently avoided or modified after shoulder replacement to protect the joint and reduce the risk of implant wear or dislocation. These include:
- Heavy lifting (especially repetitive or overhead)
- Contact sports (rugby, wrestling, competitive basketball)
- High-speed racquet sports (e.g. squash) or throwing sports
Dr Hockings will provide specific guidance based on the type of implant used, your surgical outcome, and your goals. Most patients enjoy a significant improvement in quality of life and return to a wide range of enjoyable, low-impact activities with long-term joint protection.
Frequently asked questions about reverse shoulder replacement surgery
How long does a reverse shoulder replacement last?
Modern implants used in reverse shoulder replacement have demonstrated good durability, with many lasting 10–15 years or longer, depending on activity levels and overall health. Advances in implant design and surgical technique continue to improve outcomes for suitable patients.
Will I regain full range of motion?
You may not regain full overhead range, but most patients regain enough motion for daily tasks. The goal after total shoulder replacement surgery is to have a shoulder joint that feels like a normal functioning shoulder and most patients have no pain in their shoulders and have improved function after surgery.
What’s the difference between reverse vs anatomical shoulder replacement
Anatomical shoulder replacement and reverse shoulder replacement are two different types of shoulder joint reconstruction, each designed for specific conditions.
- Anatomical shoulder replacement mimics the natural structure of your shoulder. A smooth metal ball replaces the head of the upper arm bone (humerus), and a plastic socket is placed in the shoulder blade (glenoid). This option relies on a healthy rotator cuff to move and stabilise the joint, so it's typically recommended for patients with intact rotator cuff tendons and osteoarthritis.
- Reverse shoulder replacement is used when the rotator cuff is severely torn, irreparable, or no longer functioning. In this procedure, the positions of the ball and socket are reversed: the ball is attached to the shoulder blade, and the socket is placed on the top of the arm bone. This design allows the deltoid muscle (rather than the rotator cuff) to lift and move the arm, making it a better option for conditions like rotator cuff arthropathy, massive rotator cuff tears, or failed previous shoulder surgeries.
Is reverse shoulder replacement more common than anatomical replacement?
It depends on the condition being treated. Reverse replacement is more commonly used when the rotator cuff is not functional.
Can I have a reverse replacement after a failed conventional one?
Yes, this is one of the most common indications for reverse shoulder arthroplasty.
What does reverse shoulder replacement surgery involve?
Reverse shoulder replacement is performed under general anaesthesia, often with a nerve block to assist with pain control after surgery. The key steps include:
- Incision and exposure of the shoulder joint through a deltopectoral or superior approach.
- Removal of the damaged bone and cartilage, including the arthritic humeral head and worn glenoid surface.
- Preparation and placement of the implants, with a baseplate and glenosphere on the shoulder blade and a stemmed socket on the upper arm bone.
- Securing the joint and restoring alignment, ensuring that the new joint allows deltoid-driven function.
- Closure and application of a dressing, followed by post-operative monitoring in recovery.
The procedure usually takes 1.5 to 2 hours and may require a 1–2-night hospital stay depending on your health and support at home
Are there risks or potential complications?
As with any major surgery, reverse shoulder replacement carries some risks. These include:
- Infection
- Dislocation of the prosthetic joint
- Nerve or blood vessel injury (rare)
- Stiffness or limited range of motion
- Loosening or wear of the implants over time Periprosthetic fracture
- Ongoing weakness, especially with overhead movement

If you’re experiencing ongoing pain, stiffness, or reduced movement that is affecting your daily activities or quality of life, a thorough orthopaedic assessment can help determine the cause and guide the most appropriate treatment options for your situation.
